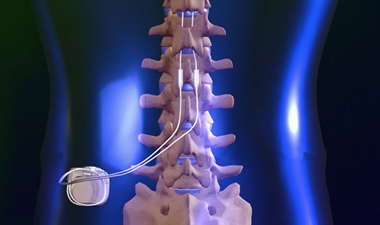
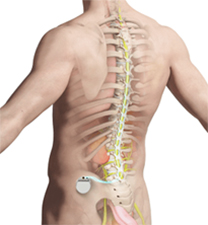
Spinal Cord Stimulators (SCS) are surgically implanted devices which transmit small amounts of electrical current to the affected spinal nerves. This innovative treatment works by changing pain signals that travel up through the spinal cord to the brain. Placed near the spinal cord in the epidural space, the spinal cord stimulator device delivers low-level electrical impulses to the spinal cord or to specific nerves that interfere with the perception of pain, especially chronic nerve pain.